Hospital Systems and Employers should be concerned about the growing number of uninsured and private payer default cost subsidies
In the healthcare market place there is an unspoken rule that when public payers receive healthcare provider service discounts for their members (Medicaid and Medicare), the cost of those unpaid for services will be passed along to private commercial and employer program payers and their members. Medicare pays providers better than Medicaid, but ultimately if you take a look at a provider’s payer case mix, it will be clear that private commercial and employer program payers are charged and pay at the highest rates. Why is this a problem? As we see from the KFF survey just released, folks are now being disenrolled from Medicaid, post Covid-19 enrollment extension protections, and for those left uninsured, 23% of right around 20 million disenrolled, all roads for any unpaid for provider services lead to the contractually vulnerable private commercial and employer program payer and their members, or will impact the bottom line of healthcare provider organizations as their bad debt write-offs go up.
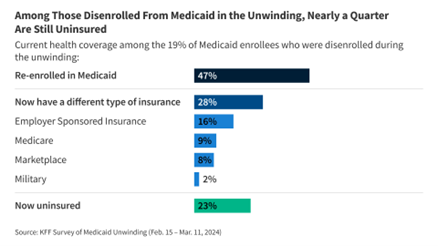
The KFF Survey of Medicaid Unwinding came out on April 12, 2024 and it says that measures put in place to allow Medicaid enrollees to remain enrolled during the Covid-19 pandemic has come to an end and millions are finding themselves, once again uninsured. While some of the disenrolled were able to re-enroll, or find coverage elsewhere 23% of the 20 million who were disenrolled are now uninsured.
Hospitals welcomed the expansion Medicaid because even though Medicaid payments are among the lowest out of their payer mix categories, at least they could receive a payment from these new expansion members who previously were making no payments at all.
If this cost is not passed along it can directly impact the net margin of hospital systems. Private commercial and employer benefit program can expect to see this cost reflected in their new contracts. These types of shifts in the market exposes private payers. Another shift that we are seeing are all the free services being offered to Medicare Advantage members this year. The cost of these free Medicare Advantage services will likely show up indirectly in private payer contracts.
The large membership payers with influence can push back during contract negotiations, but the standalone employer programs will see the pinch as their commercial hosts pass along cost to them and their employees, which means more out-of-pocket cost for individuals and families. If you were on Medicaid and find yourself uninsured, I empathize with your situation and know the trauma that you might be going through. The market can do better and the YEP card is hoping to bring that positive change to the market with urgency to address access, rising cost, affordability and sustainability. Please join us and support our efforts to make long overdue changes in the US healthcare market place.
